A new study in Nature Communications confirms what frontline workers have long known: our standards for “deadly heat” were too conservative — and the consequences are already here.
For years, climate scientists and public health officials have used a single benchmark to define the outer limit of human survivability in the heat: a wet-bulb temperature of 95°F/35°C, sustained for six hours. Breach that threshold, the conventional wisdom held, and the human body can no longer cool itself. Death follows.
A new study published in Nature Communications shows that benchmark was wrong and that people are already dying in conditions well below it.
The paper, authored by researchers from the Australian National University, Arizona State University, the University of Bern, the University of California Irvine, and the University of Sydney, applied a more accurate physiological model called HEAT-Lim to six historical heatwave events associated with high mortality. Their finding is unambiguous: non-survivable heat stress conditions have already occurred, in multiple regions, at the current level of global warming — roughly 1.1°C above pre-industrial levels.
What “Non-Survivable” Actually Means
HEAT-Lim works differently from traditional climate models. Instead of tracking a single temperature metric, it models the human body’s actual heat balance: how much heat is being generated, how much the body can shed through sweat evaporation, and at what point the system fails. The critical threshold is a core body temperature of 109.4°F/43°C, when fatal heatstroke becomes nearly inevitable.
Crucially, the model shows that survival thresholds are not fixed. They vary with both temperature and humidity, and they are considerably lower than 95°F/35°C wet-bulb for older adults in direct sun. Just one six-hour period above these physiological limits is enough to trigger irreversible organ damage even if the person survives the immediate event.
This distinction matters for how we count and understand heat deaths. The authors note that their model accounts only for physiologically-based heatstroke mortality. Cardiovascular and respiratory deaths driven by prolonged heat exposure — which represented the majority of excess mortality during events like the 2003 European heatwave — occur on top of that.
Six Events. Multiple Continents. The Same Conclusion.
The researchers examined six historical events chosen because they combined climatologically extreme temperatures with documented high mortality: the Hajj pilgrimage in Mecca (June–July 2024), a regional heatwave across Southeast Asia centered on Bangkok (April 2024), the North and Central American heat event centered on Phoenix (June–July 2023), an Australian heatwave centered on Mount Isa (January 2019), heatwaves across India and Pakistan centered on Larkana (June 2015), and the catastrophic European heatwave centered on Seville (July–August 2003).
Together, these six events were associated with more than 80,000 reported deaths. The authors suggest that the figure is a significant undercount given well-documented patterns of heat mortality underreporting, particularly in lower-income countries.
In every case, the HEAT-Lim analysis found that non-survivable conditions for older people in direct sun were reached. In the Middle East, Central America, and India/Pakistan events, more than 50% of six-hour windows during the event were classified as non-survivable for that demographic. The most consistent and dangerous conditions occurred not in the most humid locations, but in Phoenix — a finding that upends one of the field’s most persistent assumptions.
The Phoenix Finding: Hot and Dry Is Just as Deadly
Phoenix in July 2023 recorded the highest frequency of deadly conditions of any event in the study. At peak, 28% of all rolling six-hour periods exceeded physiological survivability thresholds for older people in shade. So, even people who had access to shade were at risk. The wet-bulb temperature never came close to 95°F/35°C. Relative humidity stayed at or below 20%.
This is the paper’s most consequential finding for current risk assessment frameworks. The wet-bulb temperature metric effectively assumes that humid conditions are the primary driver of dangerous heat stress, because humidity limits sweat evaporation, which is the body’s main cooling mechanism. What HEAT-Lim captures, and standard metrics do not, is that at extremely high temperatures, the capacity to produce sweat becomes the binding constraint, not the ability to evaporate it. A body trying to cool itself in Phoenix in 2023 ran out of sweat before it could run out of evaporative capacity.
The practical implication is that assessments of heat risk based on temperature alone, or on wet-bulb temperature alone, miss a large portion of the danger, particularly in arid regions, which include many of the world’s most heavily populated outdoor working environments.
Who Is Most Exposed
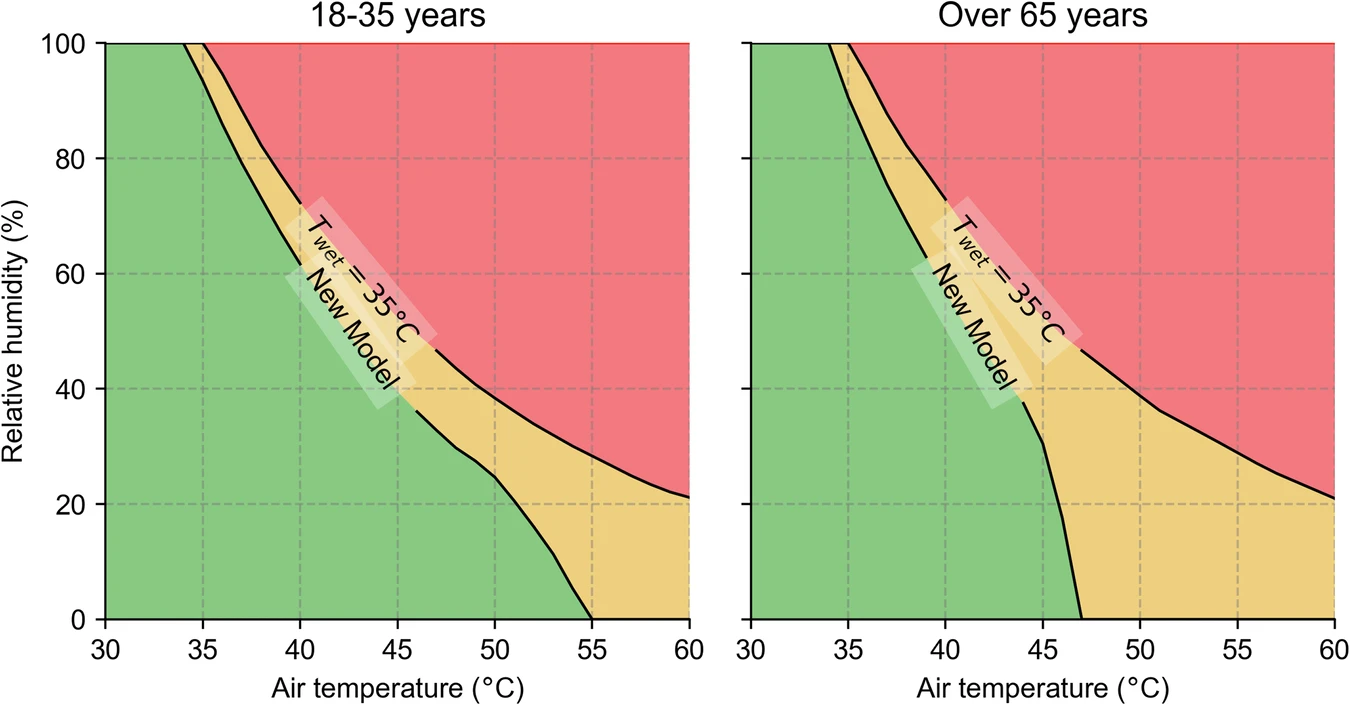
The study examines risk across two age groups — adults aged 18 to 35 and adults over 65 — and two exposure scenarios: direct sun and shade. The disparity is large and consistent.
Across all six events, older adults in direct sun faced non-survivable conditions far more frequently than any other group. In some cases (Mecca, Phoenix, Larkana) those conditions persisted for most of the day, for weeks at a time. Younger adults in direct sun also crossed non-survivable thresholds during the most extreme events. Even people seeking shade faced brief periods of lethal conditions in Phoenix and Larkana.
The authors are careful to note that these findings represent the most physiologically vulnerable among the exposed population. But they are equally clear that the populations most exposed to direct sun during these events — outdoor workers, pilgrims, people without access to adequate cooling or shade — are not statistical abstractions. They are the people who account for the deaths in Table 1 of the paper, and likely many more who were never counted.
Shade Helps. It Is Not Enough.
One of the study’s more actionable findings is that access to shade dramatically reduces non-survivable exposure across nearly all events. The maps showing conditions for older people in shade (Figure 4) are markedly less severe than those showing direct sun exposure (Figure 2) for all but the most extreme events.

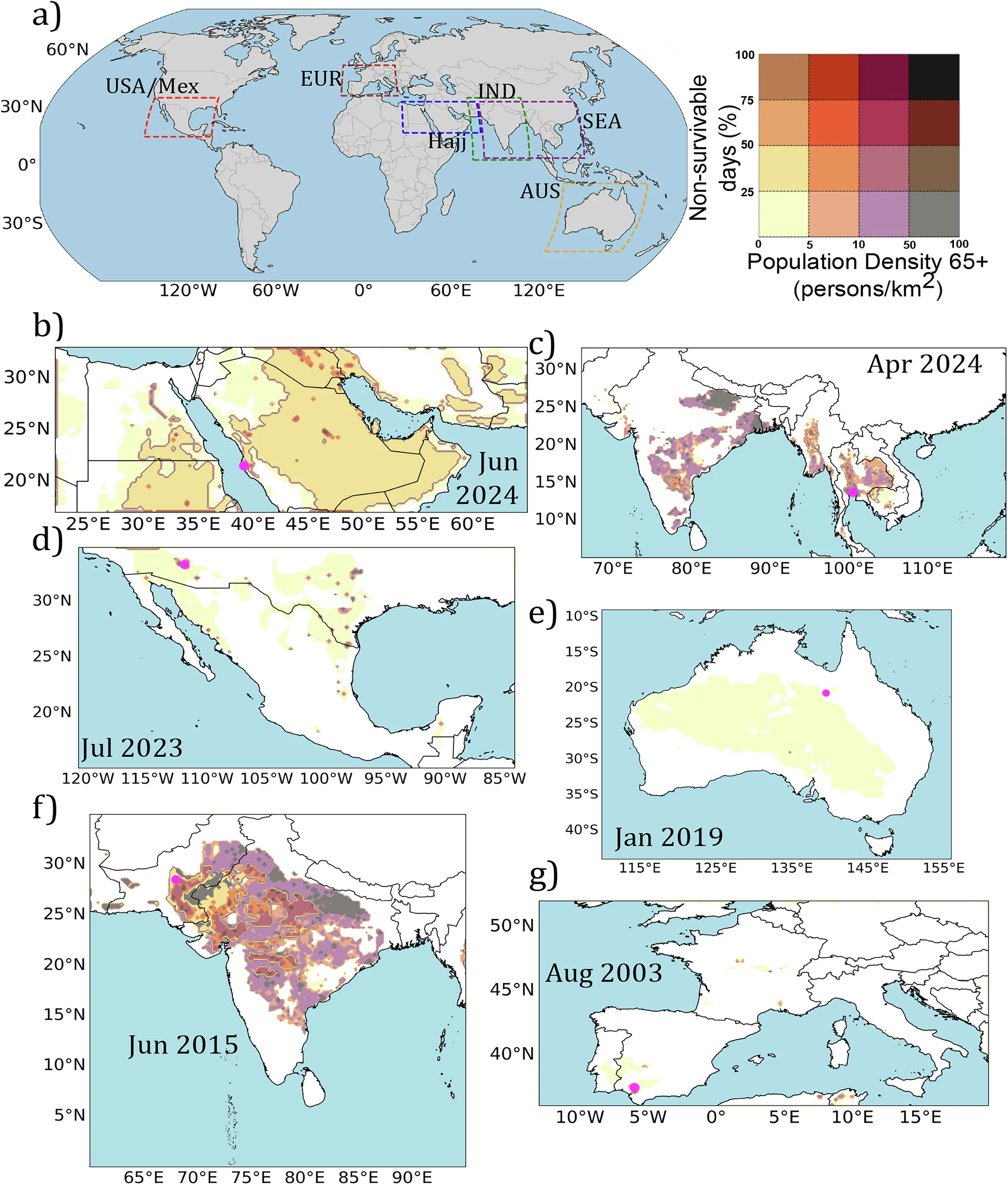
The authors frame shade access as a critical adaptation measure, and the data support that framing. But they also note that shade is not universally available — for outdoor workers, people participating in large gatherings like Hajj, and populations in communities with little green infrastructure, sustained shade access is not a given. The 28% non-survivable rate for older people seeking shade during the Phoenix event is a reminder that adaptation, while effective, does not eliminate risk under the conditions now being recorded.
The broader point the paper makes is about what adequate adaptation requires: not just shade, but fans, access to cool indoor environments, behavioral interventions, early warning systems, community-level cooling infrastructure, and enforcement of work-rest schedules. These are not exotic technologies. They are, as the authors note, viable and low-cost. The barrier is not technical. It is the failure to treat them as essential rather than optional.
Why This Matters for the Work We Do
La Isla Network has spent nearly two decades documenting what happens when workers are exposed to heat stress without adequate protection: kidney failure, heatstroke, preventable death, and communities permanently shaped by that loss. The science underlying our interventions has always pointed toward a gap between official thresholds and observed reality.
This paper closes that gap. It provides a physiological basis for what the communities we work in have already experienced: that the official markers of “dangerous” heat have consistently underestimated the actual risk to people working outdoors, particularly older workers, workers in arid climates, and workers without reliable access to shade and rest.
The findings also reinforce why systems-level interventions matter. Individual adaptation (e.g. seeking shade, drinking water) reduces risk, but cannot substitute for workplaces and supply chains designed to protect workers in the first place. The data from Phoenix and Mecca make clear that even where adaptation was available, the scale and duration of deadly conditions was enough to overwhelm it.
The world is at 1.1°C of warming. Non-survivable conditions are already occurring. Every additional degree of warming will expand their frequency, geographic reach, and duration. The question is not whether this is happening. It is whether the systems around outdoor workers will change fast enough to protect them.
Source: Perkins-Kirkpatrick, S.E., Gregory, C.H., Vanos, J.K., Baldwin, J.W., Staudmyer, H., Guzman-Echavarria, G. & Jay, O. (2026). “Deadly heat stress conditions are already occurring.” Nature Communications 17, 2590. https://doi.org/10.1038/s41467-026-70485-1
La Isla Network is a research and advisory organization protecting workers from heat stress and environmental health risks worldwide.




